
Manju B. Jayanna, M.D. Joined Our Cardiology Team
We are excited to welcome Manju B. Jayanna, M.D. to our Cardiology team located at 825 Old Lancaster Road, Suite 400, in Bryn Mawr. Dr. Jayanna
BMMSA Allergy & Immunology (formerly Suburban Allergy Associates) cares for patients of all ages with offices in Havertown, West Grove, West Chester and Narberth, Pennsylvania. Our team of board-certified allergists can help both adults and children combat allergies, asthma, and many other allergic and immunologic conditions. We offer leading-edge treatments that are safe and well-tested solutions for allergy and asthma relief. BMMSA Allergy & Immunology helps patients who have food, drug, skin, and airborne allergies manage their condition more effectively. Plus, we focus on educating patients about avoidance and develop a long-term solution to control allergies. Patients can also receive treatment for immune deficiencies, including primary immunodeficiency disease, hereditary angioedema, and sinus infections.
Our providers can assess patients for asthma by listening to their breathing and evaluating patients for symptoms like wheezing and shortness of breath. We also conduct pulmonary function tests and monitor patients with asthma. Often medications are the standard treatment for asthma, and our team educates each patient about lifestyle changes that can improve their condition.
An allergy is your body’s inability to process a particular substance, called an allergen, properly. When you have an allergy to something, your immune system perceives it as a threat to your health and reacts by producing antibodies to fight it. Because the substance is otherwise harmless, your body’s allergic response is unnecessary, but nonetheless, it can leave your skin, sinuses, airways, or digestive system inflamed.
Allergies can range from mild to severe. Some allergies can make you slightly itchy, while other allergies can actually lead to death.
There are a wide variety of allergies, including:
Some food that people are commonly allergic to include:
Symptoms of food allergies include:
Seasonal allergies are one of the more common types of allergies brought on by pollen releasing from certain plants. Seasonal allergies can give you:
The effects of seasonal allergies can feel like a cold and can leave you tired and fatigued.
Some other common allergens include:
Our team of specialists have extensive experience in diagnosing allergies. First, your doctor takes a history of your symptoms and performs a physical exam. They work with you to figure out what exactly you’ve been exposed to that might be triggering your allergies.
Once they have some idea of what might be causing your allergies, they perform a skin test or a blood test to confirm their diagnosis. A skin test involves exposing your skin to a tiny and safe amount of your suspected allergen and monitoring your body’s response to determine if the allergen produces a reaction. With a blood test, your doctor takes a sample of your blood and tests it for particular antibodies.
Your doctor works with you to determine what exactly you’re allergic to, then helps you minimize your allergies by coming up with solutions to avoid exposure to those allergens.
Medications can ease your allergy symptoms by reducing your immune system’s reaction.
For a more aggressive form of treatment, your doctor can periodically expose your body to your particular allergens, which effectively trains your immune system to stop responding to that allergen. Immunotherapy can involve injections or tablets that dissolve in your mouth, and typically takes a few years to complete.
Allergic rhinitis is an allergic reaction that occurs in and around your nasal pathways. Allergic reactions happen when your body’s immune system mistakes a non-threatening substance as harmful and tries to prevent it from entering your system by producing chemicals that swell and inflame your nasal passages, sinuses, and eyelids.
There are two types of allergic rhinitis:
People with seasonal allergic rhinitis only experience symptoms at certain times of the year, typically spring and fall. It tends to be caused by outdoor allergens like pollen.
Perennial allergic rhinitis happens all year round. It’s typically a response to indoor allergens like pet dander and dust mites.
Allergists, like the team of professionals at BMMSA Allergy & Immunology, are highly qualified to work with allergic rhinitis, due to their extensive training in the field. They pride themselves on their ability to treat and diagnose allergic rhinitis, in addition to other conditions like rhinosinusitis, conjunctivitis, and asthma.
Allergic rhinitis can cause:
The symptoms of allergic rhinitis can also leave you feeling fatigued or unable to get a full night’s rest. You might also find yourself more irritable and performing poorly in work or school when your allergies kick up.
People with allergic rhinitis are also more prone to ear and sinus infections and can develop nasal polyps or asthma if their allergies persist for too long.
The best treatment for hay fever is specific avoidance and focused treatment methods. Our team performs skin testing and devises a unique treatment and counseling plan based on your particular condition and the severity of your symptoms.
The first step in treating your allergic rhinitis is to reduce or eliminate your exposure to allergens. This can involve:
Your doctor might also suggest taking antihistamines, decongestants, steroid nasal sprays, and leukotriene modifiers to reduce your inflammation and congestion.
In more extreme cases, the team might suggest undergoing immunotherapy, which involves injecting your body with allergens at regular intervals to increase your system’s tolerance.
Anaphylaxis is a severe allergic reaction. Allergic reactions happen when your body comes into contact with an allergen. An allergen is a foreign substance that your body registers as dangerous, despite the fact that it’s not. In response to the perceived threat, your immune system produces antibodies and chemicals to prevent the allergen from entering your system.
In the case of anaphylaxis, your body so severely overreacts to the allergen that it can threaten your life.
Anaphylaxis can happen within seconds or minutes of exposure to an allergen, though it can also happen 30 minutes or longer after exposure.
Some of the symptoms of anaphylaxis include:
Without treatment, anaphylaxis can progress to anaphylactic shock, which can be fatal. Some of the symptoms of anaphylactic shock include:
If you or somebody near you is exhibiting symptoms of anaphylaxis or anaphylactic shock, call 911 immediately.
There are a few different substances that commonly trigger anaphylaxis:
If you’re prone to anaphylaxis, it’s vital to learn what you’re allergic to. Our team of experts can work with you to determine what particular allergens might trigger anaphylaxis.
Anaphylaxis is an emergency condition, and if you or someone you know is experiencing it, you need to get them to the hospital or emergency care immediately. Your emergency care physician may use several different methods to stop the anaphylaxis, including:
People that are prone to anaphylaxis need to carry emergency adrenaline medication, like an epinephrine auto-injector, at all times. This is a small, easy-to-operate syringe that can immediately deliver life-saving adrenaline to your system to counter your anaphylaxis.
Your doctor can prescribe the medication and give you tips on how to avoid anaphylaxis. They can also administer allergy testing at their clinic to help you determine what particular allergens might induce anaphylaxis, which can help you avoid exposure.
Angioedema describes a swelling in the deep layers of your skin tissue. The condition most often affects your mouth, eyelids, and genitals and often develops in conjunction with hives or welts that form on the surface of your skin.
For most people, acute angioedema occurs due to an allergic reaction to certain substances, including food and medications. Chronic angioedema can also occur due to underlying health issues or for no identifiable reason.
If you develop angioedema, you need to schedule a diagnostic evaluation to identify the root cause of your condition and the allergens that triggered the reaction. This is because angioedema and hives may be an early warning sign of anaphylaxis, a potentially life-threatening reaction that causes sudden inflammation in your airways and interferes with your breathing.
If you’re not sure what’s causing your angioedema, your provider will discuss your medical history and review your recent activities, including the foods you’ve eaten and new substances you’ve been exposed to before your symptoms started.
To determine what allergens are triggering your angioedema, the BMMSA Allergy & Immunology team offers in-office skin testing. This procedure involves pricking your skin with small amounts of suspected allergens to evaluate your body’s reaction.
In addition to lifestyle or dietary modifications to limit your exposure to allergy triggers, your provider may recommend medications that reduce swelling, such as antihistamines or anti-inflammatories.
If you’re prone to an anaphylactic reaction, your provider can also prescribe an injectable epinephrine medicine that quickly reduces airway inflammation to prevent breathing complications. They also work with you on an emergency plan to seek medical treatment at the nearest hospital or by calling 911 after an anaphylactic episode.
HAE, is a rare and potentially
life-threatening genetic condition that involves recurrent attacks of
severe swelling (angioedema) in various parts of the body, including
the hands, feet, genitals, stomach, face and/or throat. Swelling in
the airway can restrict breathing and be fatal. Episodes may be
triggered by physical trauma or emotional stress, however, swelling
often occurs without a known trigger.
Symptoms of HAE usually appear early in life, most often by age 13,
and may increase in severity after puberty. Because HAE is so rare, it
can take as long as a decade to obtain an accurate diagnosis after
symptoms are first experienced.
When untreated, an HAE attack often lasts for three days, sometimes
even longer, and many people with HAE experience three or more
swelling attacks per month. The frequency and severity of attacks vary
significantly among individuals, even among affected family members.
The vast majority of people with HAE have a genetic defect that causes
a deficiency in the plasma protein called C1-Inhibitor. HAE is also
seen in people who have normal levels of C1-Inhibitor, however,
genetic defects in other genes cause their angioedema.
What can be done
Our allergists are specialists in the care and diagnosis of this
condition. They will take a detailed history to see if you may have
this rare condition
There are new targeted medications available now for treatment and
prophylaxis of swelling caused by HAE and our specialists can help you
get the treatment that is best for you after shared decision making
and discussion.
Asthma is a condition that causes your airway to swell, narrow, and produce excess mucus. When you have an asthma attack, it can be incredibly difficult to breathe, and it can make you cough and wheeze uncontrollably.
Some of the symptoms of asthma include:
Asthma symptoms are highly variable from person to person. Some people have attacks very infrequently, while others have them quite often. Some people show symptoms all the time, while others only have issues in particular circumstances or situations.
It’s not exactly clear what causes asthma, and why some people have it and others don’t. Some of the conditions that can make you more likely to have asthma include:
If you have asthma, your condition is likely prone to certain triggers. Some of the common asthma triggers include:
In the majority of young and middle-aged people, asthma is allergy-induced and triggered by exposure to certain allergens, like pet dander, cockroach waste, mold spores, or pollen.
Our team performs a number of different evaluations to determine whether you have asthma.
They take your health history (including your family’s health history), perform a physical exam, and administer pulmonary function tests, or breathing tests. In one such breathing test, spirometry, you blow into a device that measures the speed of your airflow.
The practice also offers in-house lung function testing and can test for exhaled nitric oxide, which measures any inflammation in your lungs. They also provide rhino laryngoscopy, which enables them to make sure that your condition is actually asthma and not an anatomical issue with your vocal cords.
Our allergy specialists are uniquely suited to diagnose and treat asthma since allergies most often cause asthma. Identifying your particular allergens can help you reduce the need for asthma medications and unwanted side effects, and can help keep your asthma under control and keep you out of the emergency room.
There is no cure for asthma, but you can reduce the severity of its symptoms. Breathing exercises can help increase your lung capacity and reinforce your breathing during attacks, while rescue treatments like inhalers can provide you with quick relief when you’re in the midst of an attack. Long-term treatment, like immunotherapy, can also help reduce your asthma symptoms
Eczema, or atopic dermatitis, is a condition that causes itchiness and inflammation in patches on your skin. It can happen on nearly any part of your skin and tends to be chronic with periodic flare-ups. It’s more common in children, runs in families, and tends to happen in people who also have asthma or hay fever.
The exact cause of eczema is unclear. Some believe that it’s the result of an overactive immune system that has difficulty differentiating between foreign proteins and proteins that are part of the human body. Your immune system is supposed to attack foreign proteins, like those in bacteria and viruses, and ignore native proteins, but some believe that people with eczema have immune systems that accidentally attack their proteins, which triggers inflammation.
A number of irritants and substances can trigger an eczema flare-up, including:
For many people, certain chemicals, like those found in detergents and cleaners, can also cause a flare-up.
Eczema mainly makes your skin dry, rough, inflamed, itchy, and irritated. It can also produce:
These flare-ups can happen anywhere on your body, but they’re more common on your scalp, cheeks, back of your knees, inner elbows, and arms.
There isn’t a particular test to determine whether you have eczema. Your doctor can typically recognize it with a visual inspection.
The benefit of diagnosing and treating your eczema with an allergy specialist is that they can perform allergy tests to determine the specific triggers that are causing your eczema
Your allergist can administer a patch test to determine what allergens might be causing your eczema. They put a patch on your skin that contains a concentrated sample of a particular allergen, and then observe the reaction on your skin.
Once you know the underlying cause that’s producing your eczema flare-ups, you can treat that or eliminate it from your system to reduce your eczema flare-ups.
Hives, or urticaria, are itchy, raised welts that develop on your skin as the result of an allergic reaction to food, medication, or an irritant in the environment.
Hives can present themselves with a variety of appearances. They can be:
They can grow larger over time, change shape, and spread to different areas of your body.
Hives are typically a temporary problem that you can alleviate with allergy medications. Most hives go away within a few hours or a day, but in some cases, hives can be chronic and require medical attention.
Hives are the result of an allergic reaction. An allergic reaction happens when your immune system perceives a foreign substance as a threat and triggers a response. An immune response aims to help your body defend itself against harmful substances by releasing histamines into your bloodstream, which can cause swelling, itching, and hives.
Some of the particular allergens that can trigger a hive-producing allergic reaction include:
Hives can actually be triggered by conditions other than allergens, as well. Some other circumstances that can cause hives include:
Exposure to extreme temperatures can also trigger hives in certain people.
Our team of physicians have ample experience in treating and diagnosing hives. They can typically diagnose you from a physical exam and visually inspecting your skin.
If they suspect that your hives are the result of an allergic reaction, they might perform a skin test or blood test to determine what exact allergen is causing your hives. A skin test involves exposing your skin to various allergens and observing your body’s response. In a blood test, your doctor checks your blood for allergen antibodies to determine what you’re allergic to.
If your hives are mild and caused by an allergic reaction, you might be able to treat them by avoiding contact with the allergen. Your doctor might also prescribe antihistamines to counteract your allergic reaction.
If your hives are chronic and unresponsive to antihistamines, your doctor might recommend using oral corticosteroids to reduce your inflammatory response. If your hives are severe, an injection of epinephrine (adrenaline) or biologics might help clear them up. Biologics are drugs that contain components of living organisms or are made from living organisms. They’re typically injected, rather than swallowed orally.
The team might also recommend immunology to help you with your hives. Immunology involves injecting your body with small samples of your allergen to help your body progressively build a tolerance.
Immunodeficiency is a disorder that interferes with your body’s ability to fight off infections or diseases. A congenital immunodeficiency disorder is something you’re born with, while an acquired immunodeficiency disorder is something that you develop over time.
In a healthy body, the immune system makes antibodies to fight back against bacteria, viruses, and parasites. When you have an immunodeficiency, you aren’t able to defend against foreign invaders. As a result, you are at a much higher risk of catching bacterial and viral infections and contagious diseases.
There are two ways an immunodeficiency can interfere with your immune system’s function.
A primary immunodeficiency is the result of a genetic disorder, a condition you’re born with.
A secondary, or acquired immunodeficiency, such as AIDS, leukemia, or viral hepatitis, is the result of an infection. You can also develop acquired immunodeficiency from a disease or a toxin that attacks your body, such as:
An acquired immunodeficiency may also be the result of a poor diet and malnutrition.
After a thorough review of your personal and family medical history, we will perform a physical exam and request blood work.
Our team offers antibody tests, which involve the injection of a vaccine. Your provider then tests your blood after a few days or weeks to evaluate your body’s response to the injection. If no antibodies are present, it indicates an immunodeficiency.
Depending on the type of immunodeficiency disorder you have, your provider can prescribe medications that treat existing infections.
Antibiotics can treat bacterial infections, while viral infections may require certain antiviral drugs.
Your BMMSA Allergy & Immunology provider also recommends eating a healthy diet and getting enough sleep to strengthen your immune system. You should also avoid people who are sick to prevent developing the illness yourself.
Nasal congestion can be the result of a cold or a sinus infection, or it may be a side effect of allergic rhinitis. You can also feel congestion when exposed to dry air or environmental irritants, like cigarette smoke.
The tissues and blood vessels in your nasal passages become swollen and filled with fluids, giving you that stuffy nose sensation and making it difficult for you to breathe. Nasal congestion can also affect the way food tastes in your mouth.
While your nasal congestion and other symptoms of a cold may resolve in a few days, chronic congestion requires a diagnostic evaluation at BMMSA Allergy & Immunology.
The team at BMMSA Allergy & Immunology offers in-office testing for nasal congestion using the latest diagnostic technology to perform a rhino laryngoscopy.
A rhino laryngoscopy involves the insertion of a flexible, fiberoptic scope into your nasal passages. The slender scope has an attached camera that sends back real-time images of the inside of your nose that your doctor watches on a monitor.
This type of diagnostic procedure helps our team determine if you have obstructions in your nasal cavity that contribute to or are mistaken for chronic congestion.
If your provider suspects your persistent congestion is the result of an allergy, we offer on-site allergy skin testing to identify triggers for allergy symptoms, including congestion.
Your treatment for nasal congestion depends on the root cause of your condition. If you suffer from allergies, you may need to take over-the-counter or prescription antihistamines or other allergy medications to ease your symptoms.
BMMSA Allergy & Immunology also offers immunotherapy, a process where you receive small injections of allergens over several years that reduce your body’s reaction to your triggers.
If your congestion is the result of a sinus infection, your BMMSA Allergy & Immunology provider can provide antibiotics to clear the infection, if bacterial, and may recommend nasal sprays to moisturize your nasal passages.
To improve your ability to breathe, you can use a vaporizer or humidifier at home and may need to elevate your head when sleeping to allow fluids to drain out of the nasal cavity. Your provider can also recommend other home remedies to keep you comfortable until the congestion clears.
A sinus infection, also known as sinusitis, develops when bacteria, viruses, or molds settle into the nasal passages and cause inflammation.
While anyone can develop a sinus infection, those who have weak immune systems or asthma may be at increased risk for developing more frequent infections. Both seasonal and chronic allergies can also make you more susceptible to recurrent sinus infections.
A sinus infection often causes symptoms that are similar to a cold. Your symptoms may start out mild but worsen over time and include:
You may also notice a greenish mucus when you blow your nose.
Because the symptoms of a sinus infection are very similar to cold and allergy symptoms, it’s important that you have a diagnostic evaluation at BMMSA Allergy & Immunology to get the right treatment.
The team at BMMSA Allergy & Immunology is highly skilled in diagnosing a sinus infection. Initially, they visually examine your nose, throat, and sinus cavity, looking for signs of an active infection like:
Your provider also reviews your medical history. If you have existing allergies, they can determine if certain triggers increase your risk factors for recurrent sinus infections through allergy testing.
In some cases, you may need a sinus CT scan, which takes images of your sinus cavities, or an endoscopic evaluation where your BMMSA Allergy & Immunology provider inserts a slender, flexible tube with an attached camera into your sinus cavities to view structures in real-time. These tests can identify blockages or other abnormalities that lead to recurrent infections.
To clear the infection, we can prescribe a course of antibiotics. These medications only work if your infection is the result of a bacteria, and you need to take all the medicine as directed by your doctor to prevent the infection from returning.
If a virus or mold cause your infection, your provider can create a treatment plan using medications and home therapies to keep you comfortable until the infection runs its course. You may also benefit from decongestants to thin existing mucus or a steroid nasal spray to reduce inflammation.
In many cases, sinus infections triggered by allergic reactions can be prevented by properly treating the allergies. Our team is highly skilled in customizing treatment plans to manage chronic allergies and prevent symptoms like recurring sinus infections.
Wheezing is a side effect of underlying health issues that cause your breathing to sound like a whistle or high-pitched noise. Wheezing sounds can generally be heard when you breathe air in and out of your lungs.
Typically, any issue that blocks your airways can result in wheezing, such as:
In many of these cases, it’s inflammation in the esophagus that leads to persistent wheezing. While mild wheezing that develops along with a cold usually resolves on its own, chronic or croupy wheezing can be the first indication you have a more serious underlying health issue.
For this reason, it’s important you schedule a diagnostic evaluation as soon as possible.
The board-certified physicians at BMMSA Allergy & Immunology perform a physical evaluation of your overall health and carefully listen to the wheezing sounds to pinpoint the cause of your condition.
The team offers on-site lung function testing that measures how much and how well you can move air in and out of your lungs. This type of test can help your provider determine if your wheezing is the result of asthma.
In some cases, our team may request an exhaled nitric oxide test. This type of noninvasive testing measures the level of nitric oxide gas in a sample of your exhaled breath to determine if you have lung inflammation due to asthma.
Depending on the cause of your wheezing, we will create a treatment plan tailored to your needs.
If you have wheezing caused by asthma, your doctor can recommend short-acting and long-acting medications to treat wheezing and other asthma symptoms and prevent new ones.
If you wheeze because of an infection, you may need a course of antibiotics to clear it and prevent a worsening or the spread of the infection.
When chronic wheezing relates to a more serious lung disease, we can refer you for additional treatment with a lung specialist.
822 Montgomery Ave
Suite 318
Narberth, PA 19072
850 W Chester Pike
Suite 300
Havertown, PA 19083
Phone: (484) 270-8584
Fax: (484) 270-8799
1065 Andrew Drive
West Chester, PA 19380
455 Woodview Rd
Suite 230
West Grove, PA 19390
Phone: (610) 436-5491
Fax: (484) 270-8799

We are excited to welcome Manju B. Jayanna, M.D. to our Cardiology team located at 825 Old Lancaster Road, Suite 400, in Bryn Mawr. Dr. Jayanna

Don’t Skip Screening for Colorectal Cancer By: Jonathan Gotfried, M.D. March is Colon Cancer Awareness Month, and it’s the perfect time to highlight the importance
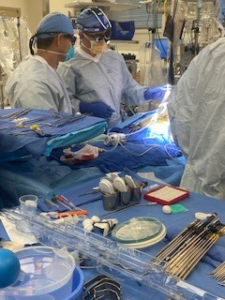
BMMSA’s Dr. Sheetal Chandhok, Main Line Health’s Dr. Basel Ramlawi and the cardiac team at Bryn Mawr Hospital, part of Lankenau Heart Institute, recently performed
Let’s get started! Answer a few basic questions to see if Jumpstart© with OPTIFAST® Program is right for you.